
Recent healthcare advancements‚ like Curbside Health’s platform with OSF HealthCare‚ and NICE guidance on dupilumab‚ highlight a focus on improved patient care.
Effective patient movement‚ as noted in Pittsburgh on February 2‚ 2026‚ is crucial for overall well-being‚ demanding careful consideration of bed positioning techniques.
Importance of Proper Positioning
Maintaining optimal patient positioning in bed is paramount to comprehensive care‚ extending beyond mere comfort. Recent healthcare innovations‚ such as the Curbside Health and OSF HealthCare partnership announced on February 2‚ 2026‚ underscore a commitment to clinical effectiveness – a goal directly supported by meticulous positioning practices;
Proper positioning directly impacts physiological functions. It facilitates effective respiration‚ circulation‚ and elimination‚ preventing complications like pressure ulcers‚ nerve damage‚ and contractures. The NICE guidance on dupilumab‚ released today‚ February 2‚ 2026‚ emphasizes targeted treatment‚ but even the most advanced therapies are less effective if basic needs‚ like comfortable and supportive positioning‚ aren’t met.
Furthermore‚ thoughtful positioning enhances patient dignity and reduces the risk of falls during transfers‚ as highlighted by concerns raised in Pittsburgh regarding patient movement. Ultimately‚ prioritizing proper positioning demonstrates respect for the patient and contributes significantly to a positive healthcare experience and improved outcomes.
Goals of Patient Positioning
The primary goals of patient positioning center around preventing complications and promoting physiological well-being. Considering recent advancements like Curbside Health’s platform with OSF HealthCare (announced February 2‚ 2026)‚ a holistic approach – integrating technology with fundamental care – is essential. This includes minimizing pressure on bony prominences to avert pressure ulcer development‚ a critical concern.
Maintaining optimal body alignment is another key objective‚ preventing nerve compression and musculoskeletal deformities. Facilitating effective respiratory function‚ particularly for patients experiencing distress‚ is also vital. The NICE guidance on dupilumab (February 2‚ 2026) highlights targeted therapies‚ but these are most effective when coupled with supportive care like proper positioning.
Finally‚ promoting patient comfort and dignity‚ while enabling access for necessary medical treatments and procedures‚ are integral goals. Addressing concerns about patient movement‚ as noted in Pittsburgh‚ reinforces the importance of safe and efficient positioning techniques.

Basic Patient Positioning Techniques
Building upon recent healthcare innovations – like those from Curbside Health and OSF HealthCare – mastering fundamental positioning is vital for optimal patient outcomes and safety.
Supine Position: Guidelines and Considerations
The supine position‚ where the patient lies flat on their back‚ is a foundational technique‚ often the default post-operative or acutely ill setting. However‚ proper execution is paramount. Head elevation‚ typically between 0-30 degrees‚ aids respiratory function and reduces the risk of aspiration‚ aligning with advancements in clinical effectiveness platforms like Curbside Health.
Careful attention must be paid to pressure points – the heels‚ sacrum‚ and occiput are particularly vulnerable. Regular turning schedules‚ ideally every two hours‚ are essential for pressure ulcer prevention‚ a concern highlighted by ongoing healthcare quality initiatives. Supportive devices‚ such as pillows under the knees‚ can alleviate strain on the lower back.
Neurological assessments should be frequently performed‚ noting any changes in sensation or motor function. Monitoring respiratory status is also crucial‚ as the supine position can compromise lung expansion. Consider the patient’s individual condition; those with cardiac issues may require lower head elevation‚ while those with respiratory distress may benefit from higher positioning.

Prone Position: Indications and Precautions
The prone position‚ lying face down‚ is a specialized technique primarily indicated for patients with severe respiratory distress‚ facilitating improved lung expansion – a goal aligning with NICE guidance on optimizing respiratory care. However‚ it demands meticulous monitoring and careful consideration.
Continuous assessment of the patient’s airway‚ breathing‚ and circulation is vital. Facial pressure points require padding to prevent skin breakdown‚ and the head must be carefully positioned to allow for unobstructed breathing. Neurological status must be frequently evaluated‚ as prolonged prone positioning can affect nerve function.
Contraindications include unstable spinal injuries‚ recent abdominal surgery‚ and severe cardiac compromise. Turning schedules are less frequent than in supine positioning‚ but regular assessment of skin integrity remains crucial. The advancements in clinical platforms‚ like those offered by Curbside Health‚ can aid in standardized monitoring protocols for prone positioning.
Lateral Position: Left vs. Right Side

The lateral position‚ lying on either side‚ is a versatile technique utilized for various clinical scenarios‚ demanding awareness of physiological implications. Choosing between the left and right side isn’t arbitrary; it’s guided by the patient’s condition and potential benefits.
Left-side positioning is often preferred for patients with cardiac issues‚ as it minimizes pressure on the vena cava‚ potentially improving venous return – a consideration mirroring the focus on optimized patient outcomes seen in healthcare advancements like those from OSF HealthCare. Right-side positioning may be favored post-stroke or for accessing the left arm for intravenous access.
Regardless of the side‚ proper alignment is crucial. A pillow between the knees maintains hip alignment‚ and the upper arm should be supported. Regular assessment of skin integrity is paramount‚ and pressure redistribution is essential‚ aligning with pressure ulcer prevention strategies. Careful documentation‚ as emphasized in effective healthcare systems‚ is vital.
Semi-Fowler’s Position: Benefits and Applications
The Semi-Fowler’s position‚ elevating the head of the bed between 30 and 45 degrees‚ offers a balance between comfort and physiological benefit. This position is frequently employed for patients requiring improved respiratory function‚ easing the work of breathing – a crucial aspect of care‚ mirroring the advancements highlighted by NICE guidance on respiratory treatments.
Benefits include reduced aspiration risk compared to flat positioning‚ making it suitable post-surgery or for those with dysphagia. It also minimizes strain on the heart‚ aiding venous return‚ and can alleviate discomfort from abdominal pressure. Applications extend to patients with mild heart failure or those recovering from certain surgical procedures.
Proper support with pillows is essential to maintain spinal alignment and prevent discomfort. Regular skin assessments and pressure redistribution remain vital‚ aligning with comprehensive patient care strategies. Accurate documentation of the position and patient response is paramount for optimal outcomes.
Fowler’s Position: High vs. Low – Detailed Comparison
Fowler’s position involves elevating the head of the bed‚ categorized as low (30-45 degrees) and high (60-90 degrees). Low Fowler’s‚ similar to Semi-Fowler’s‚ aids respiratory function and reduces aspiration risk‚ aligning with advancements in respiratory care noted by NICE. It’s ideal for patients needing moderate support‚ offering comfort while minimizing cardiovascular strain.
High Fowler’s‚ with a steeper incline‚ maximizes lung expansion and is frequently used for patients experiencing severe dyspnea or heart failure. However‚ it can increase venous return to the heart and potentially cause hypotension. Careful monitoring of vital signs is crucial.
Proper pillow support is essential in both variations to maintain alignment and prevent discomfort. Considerations include patient tolerance‚ underlying conditions‚ and the specific clinical goals‚ mirroring the focus on individualized care seen in platforms like Curbside Health’s.

Specialized Positioning for Specific Conditions
Addressing diverse patient needs requires tailored approaches‚ influenced by recent healthcare innovations like those from OSF HealthCare and NICE guidance on treatments.
Positioning for Respiratory Distress
Patients experiencing respiratory distress often benefit significantly from specific positioning strategies designed to maximize lung expansion and ease breathing. Generally‚ elevating the head of the bed – utilizing a Semi-Fowler’s or Fowler’s position – is paramount. This leverages gravity to reduce diaphragmatic pressure‚ allowing for greater chest excursion and improved ventilation.
However‚ the optimal position is individualized. Some patients may tolerate High-Fowler’s (90 degrees) better‚ while others find Low-Fowler’s (30-45 degrees) more comfortable and equally effective. Prone positioning‚ under careful medical supervision‚ can also enhance oxygenation by opening up previously collapsed alveoli‚ a technique gaining traction with advancements in respiratory care.
Continuous monitoring of respiratory rate‚ oxygen saturation‚ and the patient’s overall comfort level is essential when implementing any positioning change. Recent healthcare innovations‚ such as improved clinical effectiveness platforms‚ can aid in personalized care plans‚ ensuring the chosen position truly supports respiratory function and overall well-being.
Positioning for Post-Surgical Patients
Post-surgical positioning is critical for promoting recovery and preventing complications. Initially‚ patients often require supine positioning with minimal elevation‚ particularly following abdominal or cardiovascular procedures. However‚ early and controlled mobilization‚ including transitioning to Semi-Fowler’s‚ is encouraged to prevent pneumonia and venous thromboembolism.
Specific surgical sites dictate nuanced positioning needs. For example‚ patients undergoing hip replacement require strict adherence to abduction precautions‚ often utilizing pillows and wedges to maintain proper alignment. Careful attention to pressure points is vital‚ mirroring the focus on improved patient movement highlighted in recent healthcare discussions.
The integration of clinical effectiveness platforms‚ like Curbside Health’s partnership with OSF HealthCare‚ can streamline the implementation of evidence-based positioning protocols. Regular assessment and adjustment of the patient’s position‚ based on their surgical procedure and individual response‚ are paramount for optimal healing and comfort.
Positioning for Patients with Pressure Ulcers
Positioning is paramount in preventing and managing pressure ulcers. Frequent repositioning – typically every two hours – is essential to relieve pressure on vulnerable areas like the sacrum‚ heels‚ and elbows. Utilizing pillows and wedges strategically supports offloading and promotes circulation‚ aligning with the broader focus on improved patient care seen in recent healthcare innovations.
Lateral positioning‚ with careful attention to bony prominences‚ is often employed‚ alternating sides to distribute pressure. Micro-adjustments throughout the shift are crucial‚ going beyond simply turning the patient. Specialized positioning devices‚ such as pressure-redistributing mattresses‚ can further enhance protection.
The emphasis on clinical effectiveness‚ exemplified by Curbside Health’s platform‚ underscores the need for standardized positioning protocols. Accurate documentation of repositioning schedules and skin assessments is vital‚ ensuring consistent and proactive ulcer prevention strategies‚ mirroring the advancements discussed in healthcare today.
Positioning for Neurological Patients
Positioning neurological patients demands meticulous attention to maintain airway patency‚ prevent aspiration‚ and minimize complications stemming from immobility or altered consciousness. Side-lying positions are frequently favored to protect against aspiration‚ particularly post-stroke or following neurological surgery. Head elevation‚ often utilizing pillows or adjustable beds‚ can aid in reducing intracranial pressure‚ aligning with the focus on improved patient outcomes.
Regular repositioning remains crucial‚ but must be adapted to the patient’s neurological status and any existing limitations. Preventing contractures through proper limb support and range-of-motion exercises is essential. The integration of clinical effectiveness platforms‚ like Curbside Health’s‚ can support standardized care protocols.
Careful documentation of positioning‚ neurological assessments‚ and any adverse reactions is paramount‚ reflecting the advancements in healthcare highlighted today. Collaboration with a multidisciplinary team ensures individualized positioning plans are implemented effectively.
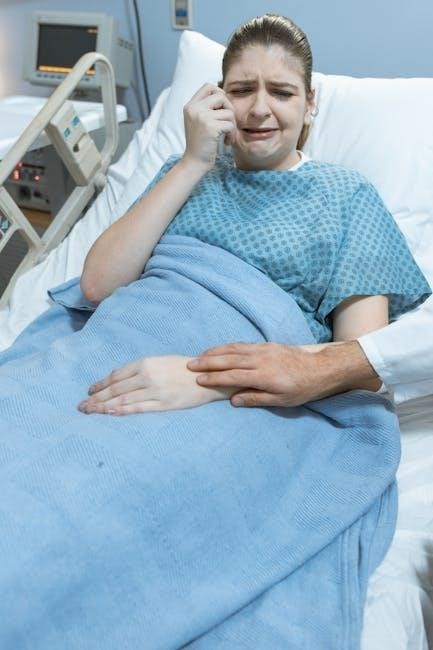
Equipment and Aids for Patient Positioning
Leveraging tools like pillows‚ wedges‚ and specialized devices—supported by platforms like Curbside Health—enhances patient comfort and safety during repositioning and prolonged bed rest.
Use of Pillows and Wedges
Pillows and wedges are fundamental tools in patient positioning‚ offering versatile support to maintain alignment and alleviate pressure points. Strategic placement is key; for example‚ a pillow between the knees in a supine position supports the natural curvature of the spine‚ reducing strain.
Wedges are particularly useful for elevating specific body parts‚ such as the head or legs‚ aiding in respiratory function or promoting venous return. Considerations include pillow firmness – softer pillows conform to body contours‚ while firmer ones provide more substantial support.
Recent healthcare innovations‚ like those discussed by Curbside Health and OSF HealthCare‚ emphasize holistic care‚ where even seemingly simple tools like pillows contribute to improved patient outcomes. Proper use minimizes the risk of complications‚ aligning with NICE guidance on optimizing treatment strategies and enhancing overall well-being.

Specialized Positioning Devices
Beyond pillows and wedges‚ a range of specialized devices assists in complex patient positioning needs. These include lateral rolling devices‚ designed to safely and efficiently turn patients‚ minimizing shear forces and reducing the risk of skin breakdown – a critical aspect of pressure ulcer prevention.

Air-fluidized beds and specialty mattresses redistribute pressure‚ offering enhanced comfort and protection for vulnerable patients. Furthermore‚ positioning aids like abduction pillows maintain hip alignment post-surgery‚ while transfer boards facilitate safe movement between surfaces.
The integration of technology‚ as seen with Curbside Health’s platform‚ suggests a growing trend towards utilizing data-driven insights to optimize positioning protocols. Aligning with NICE’s focus on effective care‚ these devices contribute to improved patient outcomes and demonstrate a commitment to advanced healthcare solutions‚ mirroring the innovations discussed in Pittsburgh on February 2‚ 2026.
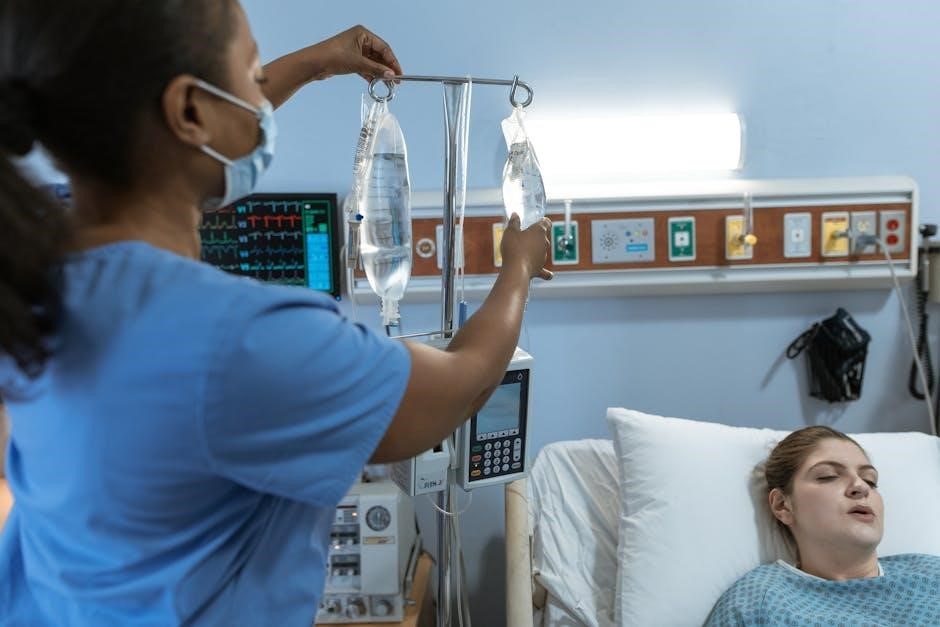
Preventing Complications from Improper Positioning
Healthcare innovations‚ like those from OSF HealthCare and NICE guidance‚ emphasize proactive care; preventing pressure ulcers‚ nerve damage‚ and contractures through diligent positioning.
Pressure Ulcer Prevention Strategies
Proactive pressure ulcer prevention is paramount in patient care‚ aligning with the advancements highlighted by organizations like NICE and the collaborative efforts of Curbside Health and OSF HealthCare. Frequent repositioning – ideally every two hours – remains a cornerstone strategy‚ distributing pressure and promoting circulation.
Utilizing pillows and wedges effectively supports vulnerable areas like heels and sacrum‚ minimizing sustained pressure. Skin assessments should be conducted and meticulously documented at least daily‚ noting any redness or breakdown. Maintaining skin hygiene and keeping it dry is also essential.
Nutritional support plays a vital role‚ ensuring adequate protein intake for tissue repair. Education for both patients and caregivers regarding proper positioning techniques and early signs of skin damage is crucial. The Pittsburgh healthcare worker’s focus on improved patient movement underscores the importance of these preventative measures.
Avoiding Nerve Damage and Contractures
Preventing nerve damage and contractures requires diligent attention to patient positioning‚ mirroring the comprehensive care approach exemplified by recent healthcare innovations like those from Curbside Health and OSF HealthCare. Prolonged pressure on nerves can lead to significant discomfort and functional limitations‚ necessitating regular position changes.
Maintaining proper body alignment is crucial; pillows and wedges can support limbs in neutral positions‚ preventing abnormal flexion or extension. Range-of-motion exercises‚ performed regularly‚ help preserve joint mobility and prevent muscle shortening. Careful attention to positioning is especially vital post-surgery‚ as highlighted in recent healthcare news.
Early mobilization‚ when appropriate‚ is a key strategy. Consistent assessment of skin integrity and neurological function is essential‚ alongside thorough documentation. The focus on improved patient handling‚ as noted in Pittsburgh‚ reinforces the need for skilled and attentive positioning practices.

Documentation and Training
Accurate records of positioning interventions‚ mirroring the detail in recent healthcare partnerships‚ are vital for continuity of care and legal protection.
Comprehensive staff education‚ like advancements from OSF HealthCare‚ ensures consistent‚ safe practices‚ improving patient outcomes and minimizing risks.
Importance of Accurate Documentation
Meticulous documentation regarding patient positioning is paramount within healthcare settings‚ serving as a cornerstone of quality care and legal defensibility. Just as advancements like Curbside Health’s platform emphasize data-driven insights‚ detailed records of positioning interventions provide a clear timeline of care provided.
Accurate charting should include the specific position utilized‚ the time of initiation‚ the frequency of repositioning‚ the patient’s skin condition assessment before and after‚ and any observed patient responses or complications. This information is crucial for effective communication among healthcare team members‚ ensuring continuity of care during shift changes or transfers.
Furthermore‚ comprehensive documentation supports risk management by demonstrating adherence to established protocols and standards of practice. In the event of adverse events‚ such as pressure ulcer development‚ detailed records can be invaluable in investigating the circumstances and preventing future occurrences. The February 2‚ 2026‚ focus on improved patient movement underscores the need for precise record-keeping.
Staff Training on Proper Positioning Techniques
Comprehensive staff training is absolutely essential for consistently implementing safe and effective patient positioning protocols. Mirroring the advancements highlighted by Curbside Health and OSF HealthCare‚ ongoing education ensures healthcare professionals possess the latest knowledge and skills.
Training programs should cover the physiological rationale behind different positions‚ proper body mechanics for caregivers to prevent injury‚ and the identification of risk factors for complications like pressure ulcers or nerve damage. Practical‚ hands-on sessions are vital‚ allowing staff to practice techniques under supervision and receive constructive feedback.
Regular competency assessments are also crucial to verify understanding and maintain proficiency. Just as NICE guidance on dupilumab reflects evolving best practices‚ positioning techniques require continuous updates. The Pittsburgh initiative (Feb 2‚ 2026) emphasizes the need for better patient handling‚ achievable through dedicated training and skill development.